The first thing I notice is the little girl’s grin. Stretched impossibly wide, it infects her face with joy. In the photograph, she’s leaning into the arms of a woman—her mother—who wears a similar smile, and her head is cocked back as if poised to launch into a fit of giggles. The two have the same haircut, a long bob with bangs. They lean into each other with ease.
The photo, taken in 1992, still radiates a soft warmth. The two of them look so happy.
Today, almost thirty years later, Kira Philips—once the little girl from the photo—sits across from me. It’s my first time meeting her, and I’m a little nervous. Sometime in the last three decades, she’s traded her bob for long, pin straight hair. Her cheekbones have become more prominent, but she still has the same warm brown eyes.
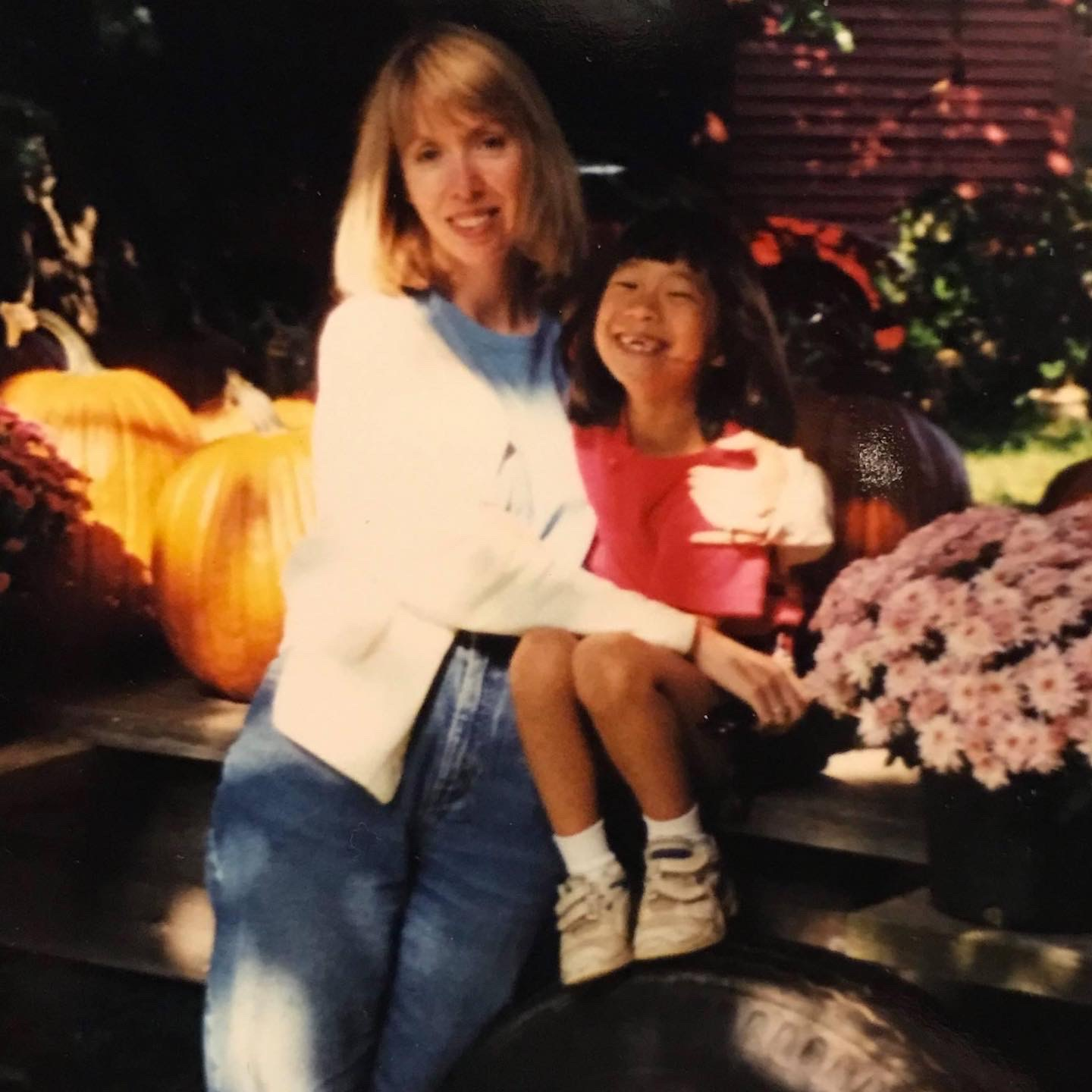
Kira and her mother Claire in 1992.
I ask her how she’s been, and she briefly grins, perhaps out of habit. But the smile hangs stagnant on her lips and doesn’t swell with the same verve as in the picture. She lets out a shuddery breath.
“You can lead the questions, and I’ll try to keep it together,” she says. “It’s been an emotional couple of days.”
This past weekend was the two-year anniversary of her mom’s passing.
I connected with Kira after finding her name in the Connecticut State Assembly’s legislation testimonial archives. Last February, she went to Hartford to testify in favor of SB 1076: An Act Concerning Aid in Dying for Terminally Ill Patients. The bill would allow terminally ill patients in the state of Connecticut the option to die by self-administering lethal medication, a procedure dubbed “medical aid in dying” by supporters and “assisted suicide” by opponents. Bills to legalize this procedure have been annually proposed—and shot down—in the Connecticut General Assembly for almost a decade.
A look into the text of SB 1076’s reveals pages of medical definitions and procedures. Co-sponsored by sixteen senators across the political spectrum, the bill stipulates the requirements for aid in dying, including that the patient must be “of sound mind,” confirmed by an attending physician; terminally ill, defined as having a prognosis of six months or less to live; and able to self-administer the medication. As I read over these documents, I wondered: What has driven this bill and the daunting procedure it represents back into the General Assembly year after year?
In September 2018, Kira’s mother Claire was diagnosed with multiple myeloma, a rare form of blood cancer. Kira tells me that her body responded “really, really poorly” to chemotherapy and that, by October, Claire was in at-home hospice, unable to get out of bed. However, after staying in hospice for three months, things seemed to take a turn for the better.
By around February, she had begun oral, non-invasive treatment and was responding well. She was in remission, her cancer cell count was decreasing, and she was able to walk and drive on her own, as well as pick up old hobbies, like painting and baking. However, Kira tells me that it was also during this time period—during the COVID-19 lockdown—that Claire bought a gun.
Kira describes that summer to me as a “heated” time in her neighborhood. With the Black Lives Matter movement in full swing and anti-vaxxer rallies regularly sweeping the streets, Claire told her husband and Kira that she had purchased the gun for protection—a decision that Kira found “uncharacteristic, especially given my parents’ political history: we’re not Republican, we don’t believe in guns.”
By the end of 2020, Claire’s body had once again stopped responding to chemo. By early 2021, there was a noticeable physical decline in Claire’s health.
Kira’s voice starts to break.
The cancer had compacted Claire’s spine and caused her to shrink “like half a foot.” There were days where Claire had to crawl up the stairs to her room because of how much pain walking caused her.
During this time, Claire had begun discussing the option of aid in dying with her husband. With aid in dying illegal in Connecticut, the two had considered moving to Vermont, where the procedure was legalized in 2013. But because of Vermont’s then six month residency requirement (which was abolished in 2023), it “wasn’t realistic” within Claire’s prognosis timeline. The family could only watch as Claire’s symptoms worsened throughout 2021.
On June 3, 2021, Claire shot herself in the head. Kira’s father found her body in the family’s backyard shed.
“None of my friends really know the magnitude of my grief,” Kira tells me. “Yes, my mom died. Yes, Mom died in a horrific way. But [she’s] not just my mom. She saved my life. She was my best friend.”
By now, tears are freely falling down her face.
“The level of trauma that this kind of death has produced for us is profound,” Kira says. “And as peaceful people, as compassionate people, as nonviolent people, it’s still unfathomable that’s how she died.”
Joining the Conversation
Since her mother’s passing, Kira has pushed for the legalization of aid in dying both in Connecticut and on a national level.
“I just can’t just live and not do something in [my mom’s] honor,” Kira tells me.
Kira’s advocacy focuses on storytelling, highlighting the emotional experiences of terminally ill individuals seeking aid in dying. In addition to regularly testifying at the Connecticut General Assembly, Kira has also participated in “They Died Waiting,” a campaign that “highlighted the stories of Connecticut residents who could have benefited from access to medical aid in dying but died without this compassionate option.”
The campaign was organized through Compassion & Choices, a national nonprofit dedicated to improving care and expanding options for people’s “end of life journeys.” According to Tim Appleton, a Senior Campaign Director of the organization, Compassion & Choices works to “improve care and expand options and end of life so everyone can chart their own end of life care journey.” Perhaps most notably, however, the organization is known for pushing for the legalization of aid in dying.
Through the non-profit, Kira also shared her mother’s story at the 2023 End of Life Symposium, a three-day conference hosted by the City of Hope Comprehensive Cancer Center in Las Vegas. According to its website, the conference is designed to educate “healthcare professionals, hospices, long-term care facilities and hospitals” on different options for end-of-life care.
“The level of trauma that this kind of death has produced for us is profound,” Kira says. “And as peaceful people, as compassionate people, as nonviolent people, it’s still unfathomable that’s how she died.”
Kira says that while telling her mother’s story is important to her, the work has also been draining. The hardest part is listening to the testimonies of those who oppose the procedure.
“It’s infuriating and also heartbreaking and also discouraging,” Kira says. “It’s like nothing—trauma or suffering—would change these people’s minds.”
Opponents of aid in dying largely fall into two categories: conservative Catholic groups who believe that suicide is a sin and progressive activists who believe that legalizing aid in dying could be weaponized against economically and socially marginalized individuals.
As Kira succinctly puts it, religious opposition, though considerable, should hold no legal sway because “separation of church and state is core to our legislation.” Still, religion—especially Catholicism—holds an undeniable, implicit influence over the state community, which has a 38% Catholic population and a history of politically active Catholic groups in the state.
In 2015, when a different variation of the bill was being considered, the Connecticut Catholic Church Conference delivered 21,000 signatures against the bill to the state legislature. The Conference’s website also currently lists “Physician-Assisted Suicide” as the first topic under their “issues” tab.
Kira tells me: “I don’t really have a problem with those religious crazies because they devalue their side when they’re spouting off [things like] ‘Suicide is a sin,’ ‘people who commit suicide go to go to hell’ and all the religious absolute garbage.”
Progressive Opposition
When I meet Joan Cavanagh, she makes two things very clear. First, her concerns about aid in dying aren’t religious. Second, while she has always been opposed to aid in dying, or assisted suicide, as opponents of the procedure call it, she only started “militantly fighting” against its legalization after her mother’s passing.
Long silver hair and a pair of black, rectangular glasses frame Joan’s face. The first time we meet, I’m intimidated by her incisive, no-frills demeanor—she’s terrifyingly articulate and emails without exclamation points. Throughout our meeting, though, I find myself warming up to her vulnerability and occasional jokes.
Joan is one of the founding members of Progressives Against Medical Assisted Suicide (PAMAS), a Connecticut-based grassroots organization fighting SB 1076 and variations of the bill that have come before it. PAMAS opposes aid in dying on the basis that its legalization would inevitably lead to its weaponization against economically, socially, and racially marginalized individuals.
It, along with other organizations, has been fighting to “provide a path for leftists and progressives who have social justice concerns” about aid in dying and to disrupt the notion that the opposition is exclusively religious and conservative. According to Joan, national conversations surrounding aid in dying legalization have been curated by large organizations like Compassion & Choices as a fight for bodily autonomy against religious conservatism—“The main funder of the opposition is the leadership of the Catholic Church,” Tim emphasized in our conversation—leaving out progressive oppositional concerns.

Progressives Against Medical Assisted Suicide protesting outside the New Haven Free Public Library in August 2021.
“The narrative that suggests that it’s only religious conservatives or right-wing Republicans who are against [aid in dying] really serves Compassion & Choices and other groups who are pushing this. They love it,” Joan says.
Joan started organizing after witnessing the way her mother, “an elderly dementia patient who was on Medicare and Medicaid,” was treated by the “medical industrial complex,” the network of corporate powers—hospitals, hospice care programs, drug companies, pharmacies, insurance companies, etc.—that form the health industry.
In September of 2011, Joan’s mother was admitted to the Yale New Haven Hospital after she began regularly aspirating and had trouble swallowing. Up until January of 2012, Joan stayed in the hospital with her mom every night and was “constantly assaulted by doctors saying, you need to let her go, you should send her off to hospice.” At the same time, however, Joan’s mother was telling her that she “wasn’t ready to die.”
Eventually, her mother’s private doctor told Joan that her mother needed a tracheostomy for her breathing. However, when Joan made the request, someone—“I think it was a nurse [but] I’m not sure. I never learned the identity of the person”—summoned an ethics committee meeting, where doctors discussed overriding Joan’s decision to continue her mother’s treatment. Joan attributes the hospital’s reluctance to continue treating her mother to financial disincentives, among other reasons.
“Medicare and Medicaid do not pay the hospital what they want for these long hospitalizations,” Joan tells me.
Historically, both Medicare and Medicaid have underpaid hospitals in reimbursement funds—only “56 percent of the amount that private insurers pay,” according to a Heritage Foundation report. According to another report published by the Commonwealth Fund, a private foundation that supports research in healthcare issues, the two health insurance programs underpaid hospitals by $24.8 billion in 2020 and, according to the American Hospital Association, by $76.8 billion in 2017.
Seeing how willing the “medical industrial complex” was to end her mother’s access to curative care spurred Joan to think about the ways that legalizing aid in dying would impact vulnerable populations such as those who are low-income, disabled, terminally-ill, and individuals of color.
“We live in a system where severely disabled people, elderly, poor, and non-white people are devalued,” Joan says. “There’s already a lot of incentive for insurance companies to go for the cheapest option of treatment.”
Joan posits that if aid in dying were to be legalized, hospitals would press patients away from curative care and into the option of aid in dying to cut costs, especially in the case of low-income individuals on Medicaid or Medicare.
The 1977 Washington v. Glucksberg Supreme Court decision also noted this potential financial incentive, stating “if physician-assisted suicide were permitted, many might resort to it to spare their families the substantial financial burden of end-of-life health care costs.”
Joan said that the corporate profit incentive, along with more circumstantial and covert pressures—familial finances, low-quality palliative care, and ableism—all lead to a reality where marginalized groups can be coerced into aid in dying. She also believes that the failure of general hospice and of palliative care is also contributing to the demand for assisted suicide.
“I heard one person speak about [supporting assisted suicide] and she was talking about how hospice had failed them and it’s clicking for me…the failure of hospice care is propelling her to support medical assisted suicide,” she said.
In November 2022, The New Yorker published an investigative piece capturing how hospice care was turning into a “for-profit hustle.” According to Connecticut Hospice, a non-profit hospice in the state and “America’s first hospice,” to qualify for hospice care, patients must be certified by two physicians, who can verify that they are terminally ill with a prognosis of six months or less to live and formally give up curative care. This is the standard for the majority of hospices around the nation. However, The New Yorker found that a growing number of for-profit hospice programs would “dupe people into the program by claiming that it’s free home health care,” illegally recruiting patients who aren’t actually terminally ill and keeping them from accessing curative care. Patients who outlived the projected hospice average of six months for profit were then “dumped” by companies. These exploitative practices have made hospices especially predatory toward low-income individuals.
Disability Rights Opposition
According to Cathy Ludlum, a disability rights activist, there is a long history of the medical industrial complex turning to assisted suicide to avoid accountability for bettering palliative care for terminally ill and disabled individuals. Cathy, a longtime Manchester, CT resident, founded Second Thoughts Connecticut, a disability rights organization fighting against the state legalization of aid in dying.
“We live in a system where severely disabled people, elderly, poor, and non-white people are devalued,” Joan says.
After a few back and forth emails, the two of us finally hop on a video call together. Cathy uses a wheelchair and joins our conversation clad in thin-rimmed glasses and a toothy grin. In the middle of exchanging introductions, Cathy turns from the Zoom camera and directs her voice towards her computer.
“Computer, wake up. Mouse click. Mouse 5…674.”
Refined by years of practice, Cathy navigates her computer exclusively using voice commands. When I ask Cathy how she started organizing against medical aid in dying, she jumps in and asks me to use the term “assisted suicide” instead.
“Medical aid in dying as a term, really, is misleading,” Cathy says. “If someone is assisting someone in their transition [to death], that would be hospice—assisting the person to be comfortable in their health, alleviating anxiety, existential concerns, and clinical concerns.”
Cathy tells me that there’s significant historical precedent for medical abuse of assisted suicide.
She points to the case of Larry McAfee as an example. In 1989, Larry McAfee, who was paraplegic and frustrated with the limitations of his life, won court permission to have his ventilator disconnected. Despite his initial decision, McAfee changed his mind after moving to a nursing home that contained specific accommodations for his disability, such as a special computer that let him contact the outside world. McAfee ended up living for six more years, until he passed from pneumonia.
According to Cathy, McAfee’s case illuminated a jarring conclusion: assisted suicide can often be a last resort that disabled individuals are cornered into because society lacks the proper accommodations—whether that’s access to technology, medicine, or caretakers—to guarantee them proper care and fulfilling lives. .
I look at Cathy, who’s sitting in her wheelchair, and her implicit argument becomes clear: If assisted suicide is legalized, my life and right to live become at risk.
Compared to other state bills that have been passed, Connecticut’s proposed legislation, with its stringent residential requirement and older age limit—21, instead of 18 like many other states—seems to be on the tighter end of aid in dying legislation.
But when I ask Cathy and Joan whether the safeguards of SB 1076—including a physician confirmation of terminal illness, a present witness who has no stake in the patient’s death, the patient needing to be sound of mind—would mitigate some of the aforementioned inequities, they presented a list of refutations. First, regulations can’t prevent covert pressure like familial pressure or a patient’s internal guilt for feeling like a burden. Second, even places like Oregon, which has legalized aid in dying for twenty-five years, admit to not having enough resources to oversee individual cases of aid in dying to check for physician negligence or coercion. Lastly, even if all the checks did initially work, Cathy argues through the cases of Oregon and Vermont, that pro-aid in dying lobbyists will often use the “bait and switch” tactic to wear down legislative safeguards over time. For instance, aid in dying was originally legalized in Vermont in 2013 under a stipulation that it could only be used by residents. However, in May, after a lawsuit filed by a Connecticut woman seeking aid in dying found Vermont’s residency requirements unconstitutional, the Vermont governor removed residency requirements. Oregon, which had passed its Death With Dignity Act with a residency requirement in 1997, also repealed its own in 2022.
In essence, according to Joan and Cathy, it doesn’t matter which guardrails were initially set with legalizing aid in dying, because there’s nothing stopping them from being worn down.
Despite the aid in dying clash’s emotional charge, its intricacies, and its interside tensions, Joan says that she has still found moments of humanity in connecting with the other side.
Once, after a bill hearing, Joan had the chance to talk to a woman testifying in support of aid in dying, who had lost her wife to a “very, very drawn-out death.” Moved by the woman’s story, Joan shared her mother’s story.
When someone’s soulmate, parent, or sibling passes, where does that love go?
“I said [to her] you know, we are not against you folks, and I really understand what it’s like to lose somebody you love, very, very painfully,” she said. “We have that same thing in common. I’ve been there. I know what it feels like.”
When Palliative Care isn’t Enough
When I meet Tyrone Biniarz, I’m greeted by a man in his late fifties, with a full white beard and deep-set voice. Tyrone—who tells me to call him Ty—is from Ellington, CT and carries himself with a frank yet warm air. Throughout the interview, he constantly reminds me: “I’m a very open person. I don’t mind you asking anything that maybe you don’t feel comfortable asking.”
In April 2016, Ty’s brother Clifford, at the time 49 years old and living in Tucson, was diagnosed with chondrosarcoma, a type of bone cancer. After complications with an initial surgery, Clifford was hospitalized in Houston for nine months. He could no longer walk on his own and lost “bowel function and control of his bladder.” Unable to live alone, Clifford moved in with Tyrone and his family in Connecticut in May 2017.
Before the cancer diagnosis, Clifford had been very active. The two brothers loved hiking the Grand Canyon “rim to rim in one hike” and going to the Indy 500 race together. However, by the time he moved in to Ty’s, Clifford couldn’t walk up a flight of stairs without assistance.
To get Clifford to his bed on the second floor of his home, Ty would secure a strap around his chest to “pull and support” his brother as he used a walker up the stairs. Despite receiving care from Ty and his family, Clifford’s mobility, agency, and life all changed irrevocably.
Since Clifford wasn’t yet a Connecticut resident or on disability, there were a lot of services he didn’t qualify for yet. SoTy, who was at the time working a full-time job, became Clifford’s full-time caretaker.
Ty learned how to take care of and clean Clifford the way a nurse would. He tended to his brother in the mornings, during his lunch break, when he’d drive home from work, and in the evenings.

Ty (left), and his brother, Clifford (right).
“I had two kids so it was [similar] to changing a baby’s diaper. But the circumstances are very different because it’s my own brother and he’s an adult, right,” Ty says. “So that was difficult.”
Though Ty was happy to help his brother out, the dynamic took “its toll financially”—and mentally. Ty went “heavily into debt” over Clifford’s medical bills. And in February 2021, Ty suffered a heart attack.
“It’s not that I had a heart attack because of him,” Ty says. “But the stress and everything in the years leading up to that… I’m sure they were contributing factors.”
During the time period leading up to Clifford’s death, Ty says that Clifford had been contemplating ways to commit suicide, because he didn’t want to “go the way [their mother] who had cancer did.” Ty knew that Clifford was communicating back and forth with someone who had access to Canadian medications. He’d contemplated hoarding all the painkillers that he was prescribed for an overdose, or overdosing through the use of fentanyl patches. Ty knew that his brother didn’t want to have to suffer for longer than necessary.
“[My brother] knew that he had a death sentence looming over his head,” Ty says.
However, none of Clifford’s plans came to fruition. He ended up being hospitalized for a cellulitis infection, where the hospital staff sent home all of the extra medication he was stashing. Afterward, Clifford was transferred into a nursing home hospice, where he passed in June 2021.
Like Kira, Ty emphasizes that his brother wouldn’t have had to suffer for so long—both physically and emotionally—if he had access to aid in dying.
However, Ty’s descriptions of the hardship that both he and Clifford faced brought me back to Joan’s argument about the failure of palliative care. If Connecticut state had immediately qualified Clifford for in-state disability provisions—if Clifford had earlier access to a colostomy bag and an in-home palliative caretaker—would he still have considered aid in dying?
Kira argues that while palliative care is important, in some cases, it’s not enough for terminally ill patients. She points to the example of her friend Amanda, who she met at the End of Life Symposium. Amanda came to support aid in dying after the death of her husband, who had bladder cancer and whose bladder had ruptured.
“[He] really, really suffered and no amount of pain medication or hospice assistance or palliative care could have alleviated his suffering,” Kira says. “That was just the manner of his cancer.”
Kira says that she doesn’t see why legalizing aid in dying and improving palliative and hospice care are mutually exclusive.
“[The opposition says] we should really focus on not killing people, [on] advancing our hospice and palliative care systems—but can’t all of those things coexist?”
I find myself returning to the photograph of Kira and Claire. Throughout our meeting, Kira described her mother to me as her best friend, her advocate, her soulmate. The fondness in her voice made me wonder: When someone’s soulmate, parent, or sibling passes, where does that love go?
I think back to something Kira told me when we first met: “I channeled my heartbreak into this work.”
Her story, along with Ty, Joan, and Cathy’s, help bring to life the intense emotions that have kept SB 1076 and its predecessors circulating in and out of the Connecticut General Assembly for almost a decade. As the next legislative year rolls around, all four of them have begun bracing themselves for the kaleidoscope of emotions the bill represents—fear, grief, and hope—and to continue the fight.
For Kira, it’s her mother. For Joan, it’s her mother and other marginalized individuals. For Ty, it’s his brother. For Cathy, it’s disabled individuals—including herself.
–Anouk Yeh is a sophomore in Pierson College and an Associate Editor for The New Journal.


